An interview with Alberto Gobbi By Maria Cristina Paganoni
“Bio-orthopaedics”, the youngest and most promising offspring of orthopaedics, can be broadly summarized as the attempt to regenerate damaged joint tissue by activating healing processes at the molecular level.
In the light of the current resurgent interest, in the national press, for knee injuries and the fate of the many patients affected (see Corriere della Sera – Salute 5th July 2009 "Artrosi. In America un severo riesame delle terapie che fa discutere. Le linee guida mettono le cure in ginocchio. Promossi a pieni voti solo movimento e dieta"), Maria Cristina Paganoni proposes an interview about the current cutting-edge research on regeneration therapies in cartilage damage, the relevant opportunities for a strategic rethinking on health policy in this area, and its impact on the social and collective thinking about issues of health and self care.
Why bio-orthopaedics?
I am a bio-orthopaedic doctor and my main area of study is cartilage repair, a field which has impressively expanded in recent years thanks to the insights provided by stem-cell research. When I began my medical career in 1983, very little of what is shared knowledge today was studied and discussed in the scientific community. Remembering the curiosity that led me to pursue this line of research, I also see that innovation in cartilage repair has shaped the entire development of my professional life. Partly as a coincidence, partly as a choice, as it so often happens, the tight connection between my life and this aspect of medical research has turned me into an enthusiastic witness of the major advancements made possible by cellular biology and bioengineering techniques in orthopaedics.
What is cartilage damage and why is it an issue in health policies?
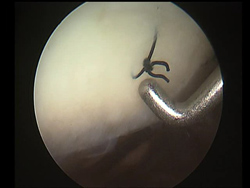
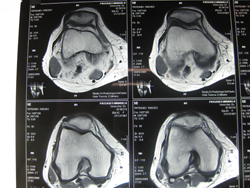
Cartilage is a thin layer of specialized connective tissue lining the joint surfaces, whose properties enable almost frictionless joint movement and protection to the underlying bone from excessive load and trauma during its movement. As this tissue is avascular, once damaged it fails to heal on its own. Current anti-inflammatory based therapies can inhibit pain caused by the damage and delay the progress of cartilage and bone loss, but unfortunately cartilage does not regenerate. This implies that, if untreated, cartilage damage only worsens over time, inevitably leading patients towards a downward path of reduced mobility, pain and eventually the need for surgical intervention. Traditional surgical procedures leave much to be desired in long-term evaluation and often lead to joint replacement. A total joint replacement may represent the only option left in the case of severe cartilage damage. It aims to improve the patient’s conditions and quality of life and often does so with good results, but it is not without its own set of problems. It is a very good option in the 60 and above age bracket, where the longevity of the artificial joint tends to match the life span of the patient. But what about young patients and active individuals who find themselves painfully limited by major constraints in lifestyle? For them the procedure marks an irreversible turning point, since it involves the possibility of multiple revision surgery in the future due to prosthesis wear and limits their activity for the rest of their lives, making them miserable in the long run.
As cartilage injuries quickly lead to arthritis, this results in a major reduction of the functional capacity of the person and represents a huge impact on social costs. Patients with impaired mobility due to bone and cartilage pathologies tend to become a lifelong burden to the healthcare system. A joint replacement is also an expensive medical procedure, as artificial prostheses are made of sophisticated and costly materials, which is the reason why they generate considerable revenues for the companies that produce them. Surgery is heavy, and recovery long and strenuous.
For all these reasons, while for the past fifty years science has focused on artificial joint replacement, over the next fifty years the challenge will be to prevent wear and tear of tissues and regenerate damaged cartilage, muscle, ligament or nervous tissue in order to restore function and delay the onset of osteoarthritis. Repairing cartilage, possibly as soon as the first lesions appear, may change people’s life for the better in the long run and, at the same time, represent a cost-effective alternative to prosthetic surgery, an issue which is particularly pressing nowadays in Western economies, faced as they are with increased health needs and dwindling budgets. In Italy alone, for example, the number of people suffering from musculoskeletal injuries has been estimated to be around 10% of the entire population.
Preventing and regenerating, not replacing
Therefore, the trend is now in the direction of preventive interventions and therapeutic solutions that can lead to the enhancement of tissue regeneration processes and the reduction of degenerative mechanisms. This is happening thanks to cutting edge research that has succeeded in jump-starting data from the lab and bringing them straight into the operating room and the physician’s office in a short span of time. I am convinced that what is currently in progress in bio-orthopaedics represents the beginning of an exciting era, which promises to be very rewarding.
In the past, patients had to live with the morbidity brought about by these problems and eventually accept the fate of a joint replacement. Today, thanks to innovative surgical and non-surgical strategies offered by bio-orthopaedics, cartilage damage can be prevented, alleviated and healed if necessary. Surgery is able to do what – only fifteen years ago – was deemed impossible, repairing cartilage with the help of bioengineered tissues. An additional, innovative and non-surgical form of outpatient treatment in the fight against cartilage damage is the use of platelet-rich plasma (PRP). This increasingly mainstream procedure entails injecting centrifuged portions of the patient’s own blood directly into the injured area, which catalyzes the body’s instincts to repair muscle, bone and other tissue. Minimally invasive and inexpensive, this technique appears to help regenerate ligament and tendon fibers and to promote the healing of damaged cartilage. Combined with proper nutrition, a cartilage specific rehabilitation program and life-style modification, it can prevent chronic and degenerative musculoskeletal disease.
Myths and Facts
The general public, however, finds it difficult to distinguish between what is myth and what is fact. Some doctors fail to fully understand and explain the benefits offered by this new biotechnology to the majority of their patients. As for the media, their often contradictory flood of information about stem-cell research either leads people to believe in unrealistic promises or generates scepticism, due to misinformation. Instead, stem-cell research applied to orthopaedics is no longer a myth, but is grounded in actual facts and encouraging data.
In spite of the successes of bio-orthopaedics which I have briefly tried to summarize above, there are still scientific and social obstacles to overcome. First, owing to the rapid pace of its development, cartilage repair is going through an experimental phase which needs to stand the test of time and produce long-term and reliable results, in order to be fully acknowledged by the scientific community. As for the specific Italian situation, though consensus is growing, not all orthopaedic doctors are unanimous in their support of bioengineering techniques, as these involve a very different approach to treating musculoskeletal pathologies.
To be fully understood and applied, this kind of innovation requires that all different stakeholders involved – researchers, doctors, health managers, patients and more generally citizens – engage in a more participatory and meaningful debate about its benefits and ultimate goals for the entire community. It is only this kind of collective engagement that will hopefully move bio-orthopaedics from the edge to the centre of patient care.